Бизнес подрал - Go2change
- Бережливое производство начинается с бережного отношения к работникам От факторов торможения - к принципам перехода
- Управление производственным снабжением фирмы Основы снабжения предприятия
- Процесс предотвращения ошибок, применяемый в Lean-системах Внедрение принципов бережливого производства на предприятии
- Классификация ценных бумаг, обращающихся на международном фондовом рынке Валютный рынок
- Методы минимизации кредитных рисков
- Секьюритизация ипотечных кредитов Секьюритизация простыми словами
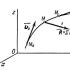
- Теорема об изменении количества движения точки Теорема об изменения количества движения материальной точки имеет вид
- Звездные величины Как перевести в звездные величины
- Какую стипендию получают белорусские студенты?
- Как узнать владельца по номеру карты сбербанка
- Бонус коды PokerStars Бонус на первый депозит pokerstars
- Как копить деньги и не тратить их: советы экспертов Почему никак не удается откладывать денег
- Регистрация и активация бонусной карты гипермаркетов карусель
- Бонусная карта Бургер Кинг — зарегистрировать и активировать через личный кабинет Карта бургер кинг личный
- Интернет-магазин обуви кари
- Вход в личный кабинет «Хоум Кредит
- Потребительский кредит по паспорту без справки о доходах от агропромкредита в
- Кредиты по паспорту Кредит наличными без справок и поручителей в день обращения
- Прохождение NieR: Automata
- Через тернии к адекватным амбициям Как формируются амбиции
- ЕГЭ: все, что нужно о нем знать Кто разрабатывает егэ
- Определение расстояний на местности
- Институты фсб россии, порядок приема
- Список образовательных учреждений мвд россии
- Переводы денежных средств с использованием карточек (их реквизитов) Что делать, если получатель не может получить перевод
- Наша стратегия Практические шаги по реализации стратегии
- Положение акционерного общества в отрасли
- Самые дорогие монеты: что искать в кошельке, чтобы заработать тысячи рублей?
- Мгновенные переводы с карты на карту сбербанка Как перекинуть деньги с одной
- Что такое биткоин простыми словами: еще одна электронная валюта или деньги нового поколения?
- Магазины-партнеры карты рассрочки Свобода от Home Credit Bank
- Магазины-партнеры карты рассрочки «Свобода» Хоум Кредит Банка
- Магазины партнеры карты рассрочки хоум кредит банк Хоме кредит банк карта рассрочки партнеры
- Виды валютных операций банков
- Скачать терминал forex club мт4 без регистрации
- Как определить время открытия бирж на рынке Форекс по московскому времени?
- Взять кредит в европейском банке россиянину Кредит в европейском банке для россиян
- Подарочная карта Gift Pass Активация подарочной карты Gift pass
- Карта гифт пасс проверить баланс
- Дистанционное обучение в аспирантуре Возможности, которые дает обучение в аспирантуре миэпп